Helping families in Greater Cincinnati and Northern Kentucky
We often get little ones with torticollis referred for physical therapy treatment to Big Blue Canopy. Providing early intervention when torticollis is first suspected leads to improved outcomes, shorter duration of treatment, and prevention of secondary complications. If left untreated, torticollis can continue to affect the whole child, contributing to development of impairments with vision, feeding, posture in sitting and walking. In later stages, if the asymmetry persists it could even lead to scoliosis, back pain, or neglect of one side of the body.
What is Torticollis?
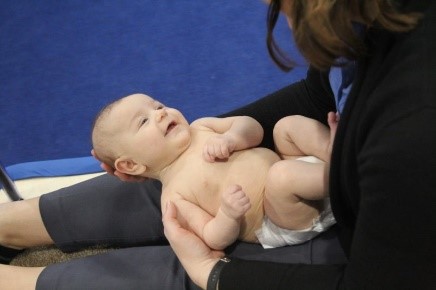
Torticollis typically presents as a head tilt towards one side with the head turned towards the opposite side. Usually, this involves the sternocleidomastoid muscle or SCM. Other muscles may include but are not limited to upper trapezius, levator scapulae, scalenes, and suboccipitals.
Torticollis can be present at birth (congenital) or acquired after birth. Both are noted to have an imbalance between the flexibility of muscle and the strength of the same muscles on the opposite side and are classified by different levels of severity. The child may demonstrate abnormal balance reactions, gross motor delay, and asymmetry through the spine and pelvis. Facial and skull asymmetry can also occur due to the tightness of neck muscles and resulting forces applied to the developing skull.
Examples:

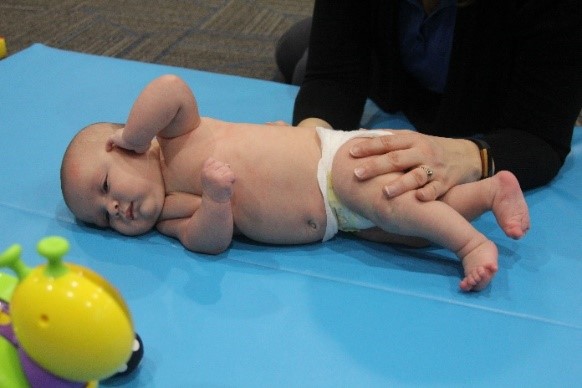
Sidebending and Rotation are opposite 
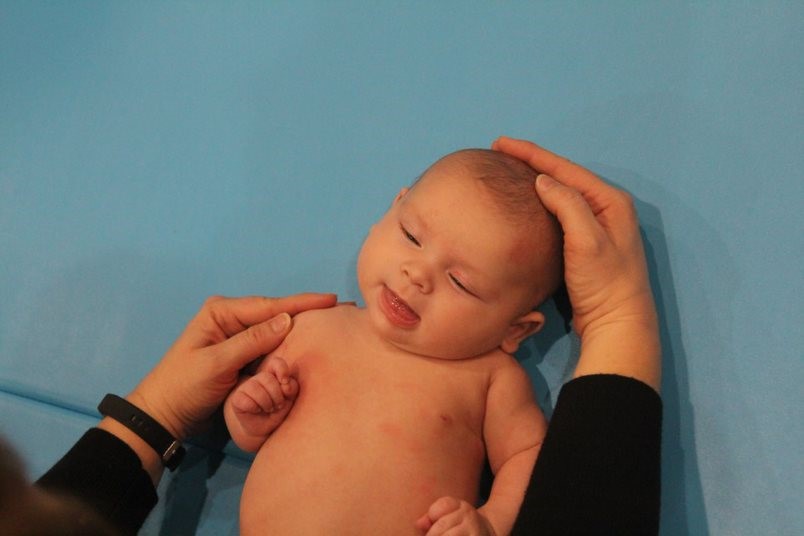
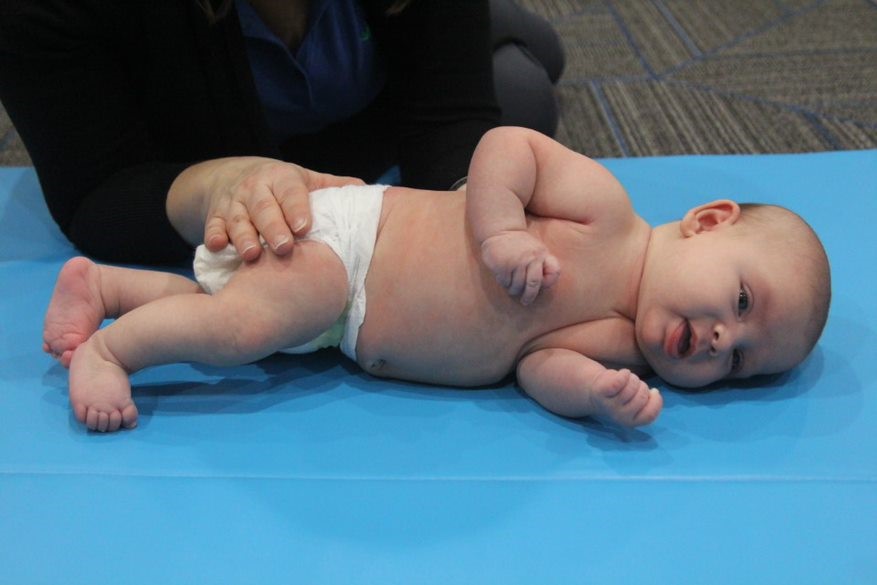
Sidebending and rotation are towards the same side
Tummy Time
Having your baby on their back for sleep and unsupervised time is the safest place for your baby to be. Following the Back to Sleep program, we saw an increase in torticollis and flat spots on babies’ heads. However, if we never place our infants on their tummies, they can have delays in their development, inability to develop strength in their necks, arms, and trunk, develop flat spots on the back of their head, and miss out on exploring the environment. Tummy time is strongly encouraged and supported by pediatricians and physical therapists during awake hours while the child is supervised.
Your doctor can advise you when it is safe for you to let your child sleep on their tummy. This is typically when the baby is older and is freely rolling independently belly to/from back. We encourage supervised, awake tummy time daily aiming to achieve 60 minutes per day. This time can be divided up throughout the day until the baby achieves strength and endurance in their neck muscles to look up at objects as well as strength in both arms. If your child has difficulty lifting their head while in tummy time, you can prop them up a rolled receiving blanket or towel, a Boppy pillow, or even over your arm or legs. As this becomes easier for them, then you can take away the support and place them directly on the floor to play with toys. Tummy time is the basis for all development!
If your child is struggling at first with tummy time, find ways to encourage this position. There are many alternatives that your therapist may be able to provide you. It is important that we help support the child to feel as tummy time as a fun place! Tummy time is a progression! Start off small and as your baby gains strength, you will see how much stronger they get as they get older. Encourage engagement with toys while they are in this position, sometimes a mirror, a light-up toy, or even you being on the floor with them will help make this position more interesting for them!
Evaluation and Treatment for Torticollis:
A Pediatric Physical Therapist is trained in evaluating your baby’s neck, head shape, postural control, range of motion, strength, and gross motor skills. During their initial assessment, your PT will identify areas to work on. The PT will establish a home exercise program and make a recommendation for treatment. Typically following the initial evaluation, weekly PT sessions are recommended. This frequency may vary based on the induvial needs of your child. Treatment and home program will include exercises to encourage head rotation actively, neck stretches into rotation and sidebending, positioning, strengthening exercises, and exercises to work on appropriate gross and fine motor skills.
What if my Baby has a Flat Spot on Their Head?
First, it is important to know that flat spots on baby’s heads have become more common with the introduction of the “Back to Sleep” program. When your child is evaluated by the Physical Therapists at Big Blue Canopy, part of their evaluation is to look for any possible asymmetries of the skull or Plagiocephaly. Our therapists are trained in anthropometric measurements of the skull to help provide our families and pediatricians with objective measurements that can be tracked monthly to assess severity and improvement of head shape. Part of the home exercise program provided by our therapists will be to educate families about how to encourage tummy time when awake and supervised and other positioning suggestions to help improve the shape of your baby’s head. If addressed early enough, flat spots may resolve on their own with correct positioning. If positioning does not improve the shape of the head, there may be a need for a referral to an orthotist who can further assess the baby’s head shape by using a low-level laser to create a 3D digital image of the baby’s head. Based on the measurements, the orthotist may recommend a cranial shaping orthoses or helmet. Your therapist can help support you during this process by listening to your concerns and answering any questions you may have about a cranial shaping orthoses or helmet.

When do we Discharge?
At Big Blue Canopy we base our decision to discharge from Physical Therapy on the criteria provided by the 2018 Evidence-Based Clinical Practice Guideline for CMT provided by the APTA:
- Passive neck range of motion within 5 degrees of the non-affected side
- No visible head tilt
- Age appropriate motor development
- Equal active movement patterns
- Caregivers understand exercises and monitoring
For more information regarding our therapy services and programs visit- www.bigbluecanopy.com
Written by Julie Horton, PT, MSPT, PCS